Aaron Trinidade, FRCS (ORL-HNS)
ENT Surgeon
Providing exceptional care for your ears, nose & throat

Helen Frankel: 07968312069
Private Secretary
Benign paroxysmal positional vertigo (BPPV)
What is BPPV?
BPPV is a condition where episodes of vertigo are caused by dislodgement of the otoconia (this is the plural of otoconium) from their normal position within the inner ear. Otoconia (also called otoliths, ear crystals or ear stones) are tiny crystals of calcium carbonate (chalk) that, together with several other factors, are important in maintaining a person’s balance.
BPPV is so called because it is Benign (self-limiting), Paroxysmal (comes on suddenly without warning), Positional (aggravated by certain head positions) and a cause of Vertigo (the sensation of spinning, as if having just stepped off a merry-go-round).
Vertigo always involves the sensation of spinning and is very different from ‘dizziness’, which is used to describe a lot of different sensations including the feeling of lightheadedness, ‘fuzziness’ or oscillopsia (the feeling of being on a ship at sea).
Though disabling at times, BPPV is not a dangerous condition.
What causes it?
People of all ages can get BPPV, but it is more common in older people. Approximately 50% of people will experience BPPV in their lifetime. Most cases occur without any precipitating events and come on ‘out of the blue’, but they can also be caused by violent head trauma, a bad viral illness or having the head in certain positions for long periods of time (for example it can happen after certain long operations when a patient has been lying flat for a long time). It can also be aggravated by other conditions affecting the inner ear, such as Ménière’s disease or labyrinthitis. Indeed, many patients with Ménière’s disease will additionally develop BPPV at some time during the course of their illness.
In the healthy ear, the otoconia lie suspended in a layer or jelly at the junction where the three semicircular canals meet and are important in helping us to sense changes in gravity and head position. When they become dislodged, they break free of the jelly layer and float around the fluid within the one or more of the semicircular canals (usually the posterior canal). They can then stimulate the canal and cause the sensation of spinning (vertigo). The canal that they are in will determine the head positions that are more likely to aggravate symptoms. BPPV occurs in one ear in most cases, but in about 10% or cases, both ears are involved.
What are the symptoms?
BPPV causes short episodes of vertigo that are aggravated by a change in the position of the head. Classically it occurs in bed when a person turns over from one side to the other, and this is by far how the most common description given by people who suffer from it. It may also occur when looking up to reach something from a cupboard, bending over to tie one’s shoes or similar situations.
Episodes of vertigo are typically brief, lasting from a few seconds to up to a minute and are rarely longer, even though it may feel that way during an attack. People are usually normal in between episodes.
When people develop BPPV, they may experience many brief episodes in a day for several days to weeks, but over time, the episodes become less and less frequent until they disappear altogether. This is because the scattered otoconia eventually work their way back to the jelly layer that they became dislodged from. In most cases, BPPV takes about 2 to 4 weeks to fully resolve naturally.
How is it diagnosed?
A description of the episodes usually gives the diagnosis and your GP or ENT specialist will spend a long time asking very specific questions about your symptoms, in particular about the presence of vertigo as opposed to other forms of dizziness. In many cases, by the time people with BPPV get to their doctor, their symptoms have fully resolved and an examination is normal. The diagnosis is therefore often made retrospectively.
The crucial test to see if the otoconia are still dislodged is called a Dix-Hallpike manoeuvre. In this test, the patient is put to sit on an examination couch with their legs up. The patient is then taken to a lying position with their head hanging backwards and turned first to one side and then repeated for the other side. If this manoeuvre causes vertigo, then the patient has BPPV. The ear on the side that the head is turned to when the vertigo starts is the ear within which the otoconia are dislodged.
How is it treated?
This depends on the current symptoms and the outcome of the Dix-Hallpike manoeuvre.
If there are no current symptoms and the Dix-Hallpike manoeuvre is negative, then it is presumed that the BPPV has self-resolved and no further treatment is needed.
If symptoms are still present and the Dix-Hallpike manoeuvre is positive, then BPPV is presumed to be present and an Epley manoeuvre is performed in an attempt to return the otoconia back to their normal position. During the Epley manoeuvre the patient is moved through a series of head and body positions that have been shown to facilitate this. Sometimes vertigo can be very severe during the manoeuvre and may cause vomiting. Most cases of BPPV will be successfully managed with 1 to 2 Epley manoeuvres. Rarely, the manoeuvre does not work.
In people who have BPPV in both ears, the worse ear (as determined by the Dix-Hallpike manoeuvre) is treated first with an Epley manoeuvre, followed by the other ear approximately 2 weeks later.
After an Epley manoeuvre is performed, it is crucial that patients follow the following rules for 5 days to prevent reversing the Epley manoeuvre:
-
No bending over at all
-
Sleep on 2 pillows
Most Epley manoeuvres fail because one or both of these rules have been broken before the 5th day.
Can BPPV come back?
Yes, about one third of patients who have had BPPV will experience it again within a 5-year period. The treatment remains the same every time.
Can I treat my BPPV myself?
Yes, many patients learn how to perform an Epley manoeuvre themselves by learning the four steps. However, before performing the procedure yourself, you should make sure that:
-
You have no neck or back problems
-
You have been shown how to properly perform the procedure by someone trained to do it
-
You know which ear is affected - this can be determined in the ENT clinic
What happens if an Epley manoeuvre does not work despite several attempts?
In the small number of cases where an Epley manoeuvre does not work, the case is reviewed to ensure that the diagnosis is correct. A CT scan of the ear can sometimes be useful in identifying other potential causes of symptoms, but do not show the dislodged otoconia if present.
If no other cause of the symptoms can be found, then surgery can be performed. This surgery is called a posterior semicircular canal obliteration, during which the posterior semicircular canal is accessed through the mastoid bone, surgically opened and plugged off, thus preventing otoconia from floating within it. The posterior canal is chosen as this is one most likely to be involved. Mr Trinidade can discuss this in more detail in the unlikely event that you need this operation.

A diagram showing the anatomy of the inner ear with 'debris' (dislodged otoconia) within the posterior semicircular canal of the inner ear. It is this debris that floats around and stimulates the canal during head movements, causing the vertigo of BPPV.

The Dix-Hallpike manoeuvre is demonstrated here. This manoeuvre is performed to test for the presence of BPPV. If BPPV is present, the patient will experience spinning as she is taken backwards.
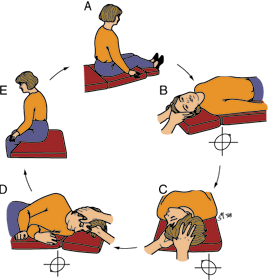
The steps of an Epley manoeuvre are shown here. The first step involves lying flat from a sitting position with the head hanging and turned towards the side of the affected ear (in this case, the right ear in Step B). Each step lasts 1 minute.